The radial nerve in the arm experiences injury or compression in Saturday night palsy. Also known as radial nerve palsy or crutch palsy. It often happens as a result of sustained pressure or compression on the nerve. Frequently occurs when sleeping or under the influence of drugs. The term “Saturday night palsy” describes a condition that is frequently observed in people who, after a night of excessive drinking, fall asleep with their arm extended over the edge of a table or the back of a chair.
The forearm, wrist, and hand muscles that control sensation and movement are under the radial nerve’s control. The wrist and finger extensor muscles may become weak or paralyzed. The elbow may be difficult to extend. And the sensation along the back of the hand and forearm may be lost when the nerve is pinched or wounded.
The course of Radial Nerve
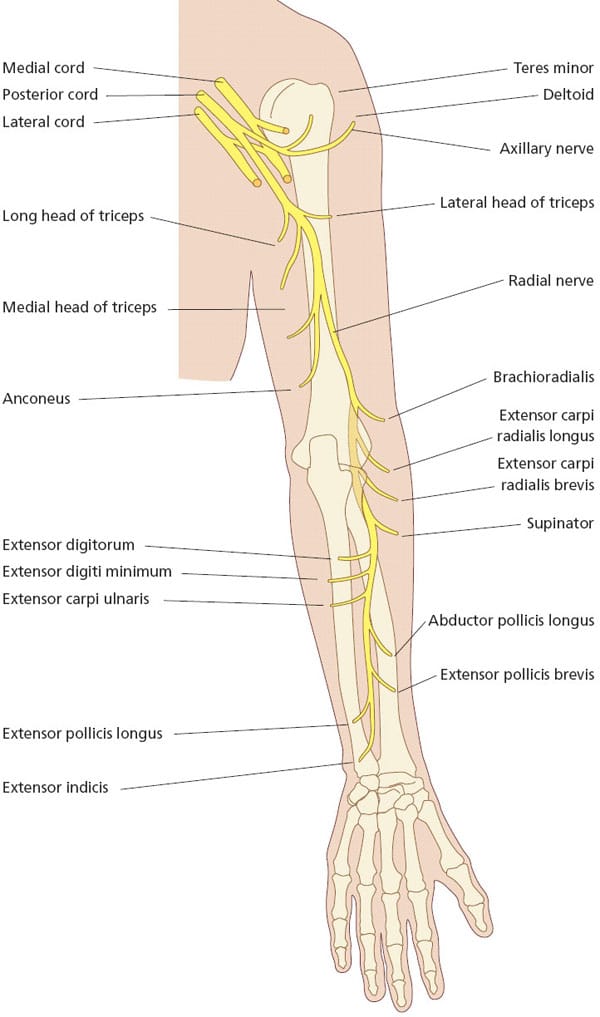
The brachial plexus, a network of nerves in the neck, is where the radial nerve’s path starts. It moves down the arm and forearm, innervating various structures along the way with motor and sensory signals.
Here is a general description of the radial nerve’s path:
1.Origin: The brachial plexus’ posterior cord, is where the radial nerve begins. Nerve root value- C5 to C8, T1.
2. Axilla: The radial nerve, axillary artery, and vein all pass through the axilla (armpit). It travels between the long and medial heads of the triceps muscle and posteriorly to the humerus bone.
3. Spiral groove: The nerve enters the spiral groove on the back side of the humerus. Between the lateral and medial heads of the triceps muscle, it curves around the humerus bone.
4. Radial tunnel: The radial tunnel, is an area created by the forearm’s muscles and fascia. It is the area where the radial nerve travels as it continues down the arm. On the lateral (outside) side of the elbow joint is where the radial tunnel is present.
5. Radial nerve branches: The nerve in the forearm emits branches, which supply the muscles and sensory areas of the forearm and hand. These branches include the superficial radial nerve. It provides sensory innervation to the skin on the back of the hand and thumb. And the posterior interosseous nerve, which innervates the muscles that govern wrist and finger extension.
6. Wrist and hand: The extensor muscles of the wrist, fingers, and thumb get motor innervation as it continues into the hand. Additionally, it gives the thumb and back of the hand sensory innervation.
Causes of Saturday night palsy
The radial nerve is repeatedly under pressure, which is the most frequent cause of Saturday night palsy. This can occur when someone spends a long time in a position that puts too much pressure on the nerve. After a night of drinking, people fall asleep with their arms resting on the back of a chair, which can cause nerve compression. This is how the term “Saturday night palsy” came to be used.
Other possible causes of radial nerve compression include:
- Prolonged leaning on a hard surface: Leaning on a hard object for an extended period can compress the radial nerve.
- Fracture or dislocation of the humerus: A fracture or dislocation of the upper arm bone (humerus) can cause injury or compression of the radial nerve.
- Pressure from casts or splints: Immobilization devices like casts or splints, when applied too tightly or in an improper position, can put pressure on the radial nerve and cause palsy.
- Traumatic injuries: Direct trauma to the upper arm or forearm, such as a fall, can compress or injure the radial nerve.
Signs and Symptoms
The main clinical signs and symptoms of Saturday night palsy, also known as radial nerve palsy or honeymoon palsy, are weakening or paralysis of the radial nerve-controlled muscles. The following list of typical signs and symptoms is clinical:
- Muscle weakness or paralysis: The forearm and hand muscles on the affected side are the predominant areas of weakness or paralysis in Saturday night palsy. The wrist, fingers, and thumb may be difficult to extend as a result.
- Wrist drop: The inability to fully extend or elevate the wrist is one of the most obvious signs. The term “wrist drop” refers to how the affected wrist may appear limp and droop downward.
- Movement issues with the fingers: People who have Saturday night palsy may have weakness in their fingers or be unable to fully stretch them. This may have an impact on activities that call for holding or moving objects.
- Numbness: In addition to muscle weakness, the affected area may experience numbness or altered sensations. Forearm, hand, thumb, and finger numbness, tingling, or loss of sensation are examples of this.
- Pain or discomfort: People who have the radial nerve compressed could feel pain or discomfort there. From a mild discomfort to a sudden, shooting agony, this can occur.
- Loss of grip power: Grip power may become less as a result of the weakened hand and forearm muscles.
- Having trouble with daily tasks: Saturday night palsy symptoms might make it difficult to write, type, button garments, or grasp objects firmly.
For a precise diagnosis and the best course of treatment, it is advisable to speak with a healthcare provider if you have these symptoms or believe you may have radial nerve palsy.
Diagnosis of Saturday night palsy
The patient’s symptoms and the results of the physical examination are generally used to make the clinical diagnosis of Saturday night palsy. The steps are as follows:
Medical history: The medical history of the patient will be examined by the healthcare professional, including any recent trauma, or injuries, that would have compressed or damaged the nerve.
Physical examination: The doctor will perform a complete physical examination. They will evaluate the forearm and hand’s extensor muscles, which are under the control of the radial nerve, for strength, tone, and mass. These include wrist drops or the inability to fully extend the fingers and thumb as indicators of weakness. In order to look for any loss of sensation, they could additionally assess sensory function in the affected area.
Provocative tests: In some circumstances, the healthcare professional may carry out provocative tests to evaluate the radial nerve’s functionality. (Discussed below)
Nerve conduction studies (NCS): To assess how well the nerves are working, NCS measures the electrical activity in the nerves. It might aid in locating the exact location and degree of nerve compression or injury.
EMG: Electromyography is frequently done in conjunction with NCS. This can assist in identifying whether there is nerve injury or whether the muscles are working appropriately.
Imaging tests: In some cases, imaging tests such as X-rays, ultrasound, or MRI scans may be helpful. These tests can help identify any underlying fractures, dislocations, or masses that could be compressing the radial nerve.
Provocative tests for Saturday night palsy
It is possible to diagnose Saturday night palsy (radial nerve palsy) by using provocative tests to evaluate the radial nerve’s functionality. In order to mimic or aggravate the symptoms, these examinations entail moving or stressing the afflicted arm. Here are a few typical provocative tests:
- Resistive wrist extension: The patient will be asked to actively extend their wrist against resistance during the wrist extension test. A positive test result could be caused by the patient’s inability or weakness to extend their wrist in Saturday night palsy.
- Resistive thumb extension: The patient will be asked to actively extend their thumb against resistance during the thumb extension test. The radial nerve may not be functioning properly if the thumb is weak or difficult to extend.
- Finger extension test: The patient will be asked to actively extend their fingers against resistance during the finger extension test. The radial nerve may be damaged if there is weakness or difficulty extending the fingers.
- Tinel’s sign: Usually near the back of the upper arm or elbow, the healthcare provider may lightly tap or percuss along the radial nerve’s route. This may indicate nerve irritation or compression if it causes tingling or an electric shock-like sensation that spreads down the forearm and into the hand.
- Pressure provocation test: The medical professional may gently press over specific locations where the radial nerve travels, such as the radial tunnel or the spiral groove of the humerus. When pressure is applied, symptoms may worsen or become more painful, which may indicate radial nerve involvement.
Differential diagnosis
- Other nerve compressions: Conditions such as carpal tunnel syndrome, cubital tunnel syndrome, or thoracic outlet syndrome can cause similar symptoms to Saturday night palsy. These conditions involve compression or irritation of different nerves in the upper extremity.
- Brachial plexus injuries
- Peripheral neuropathy
- Musculoskeletal injuries
- Radiculopathy
Treatment of Saturday night palsy
The underlying reason and the severity of Saturday night palsy, determine the appropriate course of treatment. Here are a few typical treatment methods:
Observation and conservative treatment: The healthcare professional may advise observation and conservative treatment in minor situations where the nerve compression may go away on its own. This entails refraining from actions that can make the symptoms worse and giving the nerve time to heal naturally.
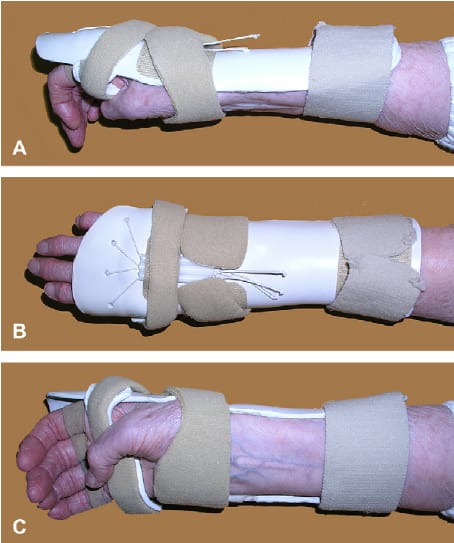
Immobilization: Splinting the injured arm helps prevent further damage to the radial nerve and speeds up recovery.
Physical therapy (Discussed below separately)
Anti-inflammatory medications may treat pain and inflammation brought on by nerve compression. Additionally, drugs like gabapentin or pregabalin may be advisable if there is neuropathic pain or persistent discomfort.
Surgical intervention may be required in rare instances of severe or persistent nerve compression. By removing any objects or masses that are compressing the nerve or by treating any damage to the nerve, surgery seeks to decompress the affected nerve. The level of nerve injury and the underlying cause are two criteria that affect whether to have surgery.
Assistive devices: In some circumstances, using braces, splints, or orthotics to support the injured arm and help with functional activities may be advisable.
The healthcare provider will choose the precise treatment strategy after thoroughly evaluating each patient’s circumstance. It’s crucial to speak with a medical expert to get a proper diagnosis and course of treatment for Saturday night palsy. To promote the best possible recuperation, they can make tailored recommendations and check on the condition.
Physiotherapy management
The rehabilitation for those with Saturday night palsy heavily depends on physical therapy. Restoring muscle strength, enhancing ROM, enhancing functional abilities, and promoting nerve healing are the main objectives of physical therapy.
Following are a few typical physical therapy techniques for Saturday night palsy:
- ROM Exercises: Exercises to restore and enhance the range of motion in the affected arm, wrist, and hand are provided by physical therapists. To maintain or recover flexibility, these workouts could involve passive or active ROMs.
- Strengthening activities: To regain muscle strength in the injured arm and hand, strengthening exercises are crucial. Physical therapists will create an individualized progressive strengthening program for the patient that may include resistance band, weight, or therapeutic equipment exercises.
- Techniques for sensory re-education may be applicable if there is any loss of sensation or alteration of sensation in the afflicted area. Through a variety of sensory stimulation activities, these methods seek to enhance sensory awareness and discrimination.
- Functional training: Rehabilitation aims to assist patients to regain their independence in daily activities by enhancing their functional abilities. Physical therapists will work with patients to establish methods and modifications for carrying out particular functional tasks, like, taking care of one’s appearance, writing, and using utensils.
- Techniques for managing pain: Modalities, such as heat or cold therapy, or manual therapy techniques, to help control pain and discomfort brought on by radial nerve palsy.
Exercises for Saturday night palsy
It’s essential to speak with a physical therapist before beginning any exercises so they can accurately assess your condition and create a customized exercise plan for you. Given that, the following general activities may be useful in the treatment of radial nerve palsy:
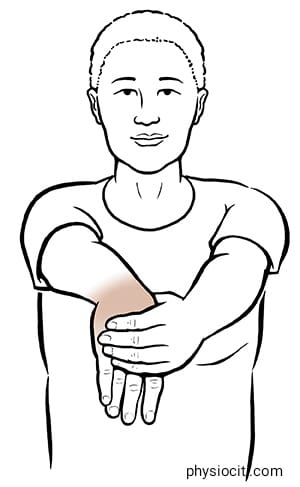
- Stretching the wrist involves extending the affected arm in front of you with the palm down. To feel a stretch in the forearm, gently bend your wrist backward with your other hand. Repeat the stretch three times while holding it for 15 to 30 seconds.

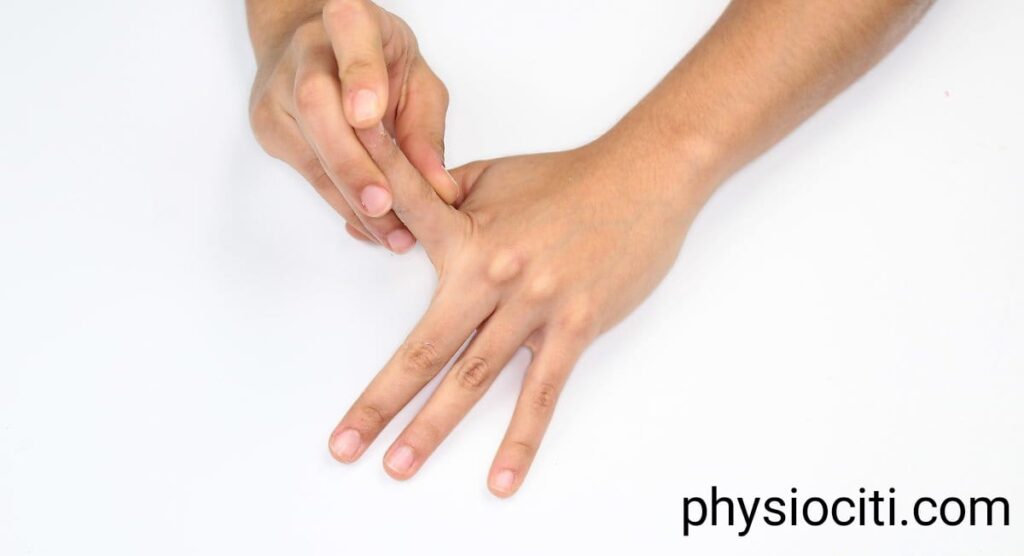
2. Finger and thumb extension exercises: Place your affected hand flat on a table with your fingers and thumb spread apart. Slowly lift and extend each finger and the thumb one at a time, focusing on the movement at the joints. Repeat this exercise for 10-15 repetitions on each finger and thumb.
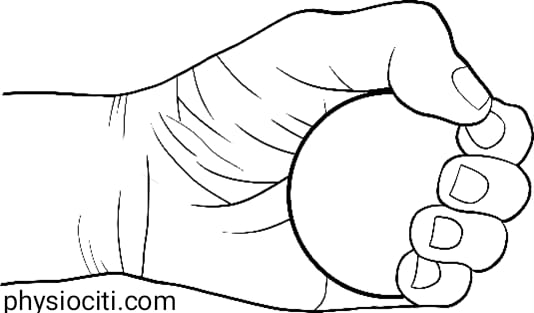
3. Grip strengthening exercises: Squeeze a soft foam ball or a therapy putty in your affected hand, focusing on activating the muscles responsible for gripping. Hold the squeeze for a few seconds and then release. Repeat this exercise for 10-15 repetitions.

4. Forearm pronation and supination exercises: Sit or stand with your affected arm resting on a table or your thigh. Hold a light dumbbell or a small weighted object (such as a hammer) in your hand. Keeping your elbow bent at 90 degrees, slowly rotate your forearm inward (pronation) and then outward (supination). Perform 10-15 repetitions in each direction.

5. Nerve gliding exercises: These exercises help to mobilize and release any adhesions or restrictions along the radial nerve. One example is the “piano-playing” exercise: Extend your arm in front of you with the palm facing down, then flex your wrist and fingers like you are playing the piano. Slowly return to the starting position and repeat.

Key Points:
Causes: Prolonged compression of the radial nerve, is a common cause of Saturday night palsy. Trauma, fractures, dislocations, or direct nerve injury are additional causes.
Symptoms: Weakness or paralysis in the radial nerve-controlled muscles, such as the wrist, finger, and thumb extensors, is the most typical sign of Saturday night palsy. It’s also possible to have sensory loss or altered sensation.
Clinical characteristics: A clinical examination may show a lack of strength or the inability to perform specific movements, such as wrist, finger, or thumb extension. Sensory tests may reveal a loss of sensation or a reduction in sensitivity in particular radial nerve-supplied locations.
Diagnosis: Diagnosis is based on the patient’s medical history, clinical examination, and the exclusion of other potential causes. To evaluate nerve function and locate the site of nerve compression or injury, further tests may help, such as nerve conduction studies (NCS) and electromyography (EMG).
Treatment: The degree and underlying cause of Saturday night palsy will determine the appropriate course of treatment. It is frequently advised to use conservative care, which includes observation, immobilization, and physical therapy.
Prognosis: With the right treatment, most Saturday night palsy cases recover within a few weeks to months. Depending on the severity of the nerve damage and other unique conditions, the recovery of nerve function and muscle strength may vary. Rehabilitation and functional recovery are greatly enhanced by physical therapy.
It’s crucial to speak with a medical expert for a precise diagnosis and effective treatment of Saturday night palsy. To provide the best possible rehabilitation, they can make personalized recommendations and check on your development.
ALL THE BEST!
